Christmas was great. It was so nice to be home celebrating together. We had a nice dinner, played games with the kids, and just relaxed and hung out. Low key and absolutely perfect!
B is doing pretty well at home. He seems much happier and more contented. He smiles alot and has started cooing a little too. It's awesome to be able to interact with him now! A nurse from VNA comes every other day to take blood for CBC's, check his vitals, and monitor his growth. He's got a long way to go but is up to 7 pounds 14 ounces now. It's crazy to think that he is almost four months old and still wearing Newborn clothes -- such a little peanut!!
We're adjusting pretty well too I guess. Its definitely exhausting though. Right now, I'm the only one who knows 100% of his care so it's a lot of pressure. Tim is learning more and more and trying to give me a break but once he goes back to work he won't be here to help much. I'm trying to find out if B would qualify for any kind of nursing or respite care to help me out but it's tough figuring out where to start. Our pedi said maybe the hospital social worker, who said they can't help since he was now discharged and recommended we ask Early Intervention but we haven't even heard back from EI since B's referral. Frustrating! I'm sure I'll figure it out eventually.
The coming weeks will be pretty busy. Brady has transfusions 2-3 times a week, IVIG weekly, and an average of two other medical appointments a week. He is followed by surgery, lung center, hematology, feeding clinic, nutrition, developmental clinic, cardiology, and neuro & growth...basically, a small army of doctors and specialists.
On Jan 3rd he is having a clinical swallow evaluation. I'm really looking forward to it because it's the first step toward allowing him to start back on oral feedings. He has not had a bottle since the beginning of November. I miss the normalcy of snuggling my baby and feeding him his bottle. I really hope that working with the speech pathologists in the feeding clinic can get him back on track but there is a good chance he will never take a bottle and could take a very long time to learn how to eat and drink anything at all. Only time will tell I guess. I'm also hoping the swallow study will show what is going on with his reflux. Supposedly the Nissen wrap stops him from refluxing but I can definitely hear it happening still and it seems to be occurring more and more frequently. Last night he had a pretty scary episode where it seemed like he was trying to vomit (which he can't because of his nissen) and it caused him to have trouble breathing. His O2 sats dropped and he had some color change. The whole thing lasted about 8 terrifying minutes. When I called the hospital and spoke with the pulmo on call he didn't seem too concerned but he isn't B's regular doctor and doesn't really know B's complexities so I'm anxious for Dr. Sheehan to get back from vacation. I think more needs to be done to manage his GERD still and that taking him off all but one reflux med was a mistake. Guess we'll see what he thinks!
Friday, December 28, 2012
Tuesday, December 25, 2012
Saturday, December 22, 2012
Mystery Diagnosis
A while back, way back on caringbridge actually, I mentioned that the genetic lung disorder both B and Ethan have had been featured a few years ago on the TLC show "Mystery Diagnosis". Today I noticed the rerun was on so I taped it and posted it to my youtube in case any of you may want to watch it. The quality isn't the best but you get the point. Here's the link:
Mystery Diagnosis Episode
Mystery Diagnosis Episode
Wednesday, December 19, 2012
A minute to reflect
Yesterday marked three months since Brady's birth. As I sit here sipping my coffee and enjoying the quiet of our usually chaotic home I can't help but reflect on the last three months.
Awhile back, maybe a month into B's hospital stay, as I was leaving the house one night Miranda nonchalantly asked me a question that broke my heart.
She asked "Mommy, what day will I see you again?"
It wasn't a complaint. She wasn't upset. This was her new normal. She knew that Brady needed me. There was acceptance in her voice. It was that accpetance that killed me. My little girl has always come home from school to her mommy, every day. And now, she didn't even know when she would see me again.
Since Brady's birth there have been a lot of moments like that one, fleeting moments that leave my heart aching. Ethan now clings to me every minute he's home. Kristyna looks surprised every time she walks in the door and finds me here. It's still surreal to think about what our family has endured already, is dealing with now, and will continue to face in the future. Kristyna, Miranda, and Ethan have had their entire world turned upside down. They've been shuffled from house to house and person to person, and lost any sense of routine and normalcy, and yet they take it all in stride. They accept their new brother and all that comes along with him. They welcome him with open arms. Why? Because above all else we are a family. And as I tell my kids all the time. . .family is forever!
Awhile back, maybe a month into B's hospital stay, as I was leaving the house one night Miranda nonchalantly asked me a question that broke my heart.
She asked "Mommy, what day will I see you again?"
It wasn't a complaint. She wasn't upset. This was her new normal. She knew that Brady needed me. There was acceptance in her voice. It was that accpetance that killed me. My little girl has always come home from school to her mommy, every day. And now, she didn't even know when she would see me again.
Since Brady's birth there have been a lot of moments like that one, fleeting moments that leave my heart aching. Ethan now clings to me every minute he's home. Kristyna looks surprised every time she walks in the door and finds me here. It's still surreal to think about what our family has endured already, is dealing with now, and will continue to face in the future. Kristyna, Miranda, and Ethan have had their entire world turned upside down. They've been shuffled from house to house and person to person, and lost any sense of routine and normalcy, and yet they take it all in stride. They accept their new brother and all that comes along with him. They welcome him with open arms. Why? Because above all else we are a family. And as I tell my kids all the time. . .family is forever!
Saturday, December 15, 2012
68, 33 & other numbers...
Wednesday, December 12, 2012
It takes a village...
...or one really determined mommy!
The amount of coordinating that has gone into getting B home this week is absolutely crazy. Seriously, small countries are probably run with less effort, lol.
Yesterday the home supply company for B's oxygen was having a problem billing his insurance. They called me and said that IHA is saying Brady does not have coverage and I need to call them. So I called IHA and they told me they never received any information on Brady, didn't even know we had had a baby. Great. Turns out Tim's HR person misfiled Brady's enrollment forms and they were never submitted. I spent the entire morning on the phone with the benefits manager straightening everything out and getting him enrolled but he is officially covered under IHA, thank goodness!!
So last night the company delivered B's oxygen compressor and portable tanks. This afternoon they came and showed me how to use the compressor, the tanks, his pulse oximeter and also to go over infant CPR. I tried to set up delivery of his feeding pump & supplies and his IV pump & PICC supplies but due to crazy issues with insurance coverage they won't deliver "home care" supplies before his discharge papers are signed. So Friday will be even more hectic trying to get everything situated at home as quickly as possible. I'm nervous because B gets a continuous feed through a pump. If VNA is late delivering he will get behind on his nutrition requirements and because he's already so far behind growth wise, that's a big deal for him. Fingers crossed VNA comes when they say they will.
It's been quite a task setting him up with all of his outpatient appointments, getting all his meds filled, coordinating his homecare nursing, and all the supplies he'll need. He'll be at the hospital for blood transfusions as needed, most likely every 2-3 days, he'll get IVIG in the infusion clinic every Thursday and he'll need to be followed by: lung center, hematology, cardiology, surgery, GI, feeding clinic, neurology, hearing clinic, and early intervention -- that's A LOT of appointments! Right now, Brady is a full time job!! haha...But it will all be worth is when we get to snuggle him and all be together at home. I can't wait!

The amount of coordinating that has gone into getting B home this week is absolutely crazy. Seriously, small countries are probably run with less effort, lol.
Yesterday the home supply company for B's oxygen was having a problem billing his insurance. They called me and said that IHA is saying Brady does not have coverage and I need to call them. So I called IHA and they told me they never received any information on Brady, didn't even know we had had a baby. Great. Turns out Tim's HR person misfiled Brady's enrollment forms and they were never submitted. I spent the entire morning on the phone with the benefits manager straightening everything out and getting him enrolled but he is officially covered under IHA, thank goodness!!
So last night the company delivered B's oxygen compressor and portable tanks. This afternoon they came and showed me how to use the compressor, the tanks, his pulse oximeter and also to go over infant CPR. I tried to set up delivery of his feeding pump & supplies and his IV pump & PICC supplies but due to crazy issues with insurance coverage they won't deliver "home care" supplies before his discharge papers are signed. So Friday will be even more hectic trying to get everything situated at home as quickly as possible. I'm nervous because B gets a continuous feed through a pump. If VNA is late delivering he will get behind on his nutrition requirements and because he's already so far behind growth wise, that's a big deal for him. Fingers crossed VNA comes when they say they will.
It's been quite a task setting him up with all of his outpatient appointments, getting all his meds filled, coordinating his homecare nursing, and all the supplies he'll need. He'll be at the hospital for blood transfusions as needed, most likely every 2-3 days, he'll get IVIG in the infusion clinic every Thursday and he'll need to be followed by: lung center, hematology, cardiology, surgery, GI, feeding clinic, neurology, hearing clinic, and early intervention -- that's A LOT of appointments! Right now, Brady is a full time job!! haha...But it will all be worth is when we get to snuggle him and all be together at home. I can't wait!

Monday, December 10, 2012
Hurry up Friday!
-Orison Swett Marden
Brady's doctors say he will be able to go home Friday
(as long as he behaves himself and doesn't pull anything new this week)
This mommy is over the moon happy :) :)
Saturday, December 8, 2012
Hope
Brady has been cleared by nutrition, surgery, and respiratory to GO HOME! Hematology says they are hoping to discharge him by the end of the week!!!
He'll come home with a lot of care - G tube, PICC line & IV meds, and oxygen - and he'll need to come back here every other day to be transfused but he'd be home. I'm crying just typing this. It would be an absolutely incredible blessing to bring him home and be together as a family. If I've learned anything though, it's that nothing is set in stone. Things don't always go as planned and he may not come home this week but it is so wonderful to know it's even a possibility.
And so, I have hope.

He'll come home with a lot of care - G tube, PICC line & IV meds, and oxygen - and he'll need to come back here every other day to be transfused but he'd be home. I'm crying just typing this. It would be an absolutely incredible blessing to bring him home and be together as a family. If I've learned anything though, it's that nothing is set in stone. Things don't always go as planned and he may not come home this week but it is so wonderful to know it's even a possibility.
And so, I have hope.

Tuesday, December 4, 2012
Could it be RSV?
B started sneezing and coughing during the night Sunday night. This morning they sent out a respiratory screen and this afternoon he had a chest xray. We're keeping our fingers crossed that he just has a run of the mill cold but with it being the start of RSV season the docs are concerned. So far, he's managing okay, he's just boogery and slightly tachypnic.
He also started with some yellow discharge from his G tube site yesterday. They sent off a culture for possible infection and we're waiting for those results too.
We need to get this kiddo out of the hospital. The longer he's here the more he is exposed to and he's already so weak :(
On a positive note, since his IVIG on Thursday he has gone almost 3 days before needing a transfusion. Its still not near being under control but 3 days is certainly better than EVERY day!
He also started with some yellow discharge from his G tube site yesterday. They sent off a culture for possible infection and we're waiting for those results too.
We need to get this kiddo out of the hospital. The longer he's here the more he is exposed to and he's already so weak :(
On a positive note, since his IVIG on Thursday he has gone almost 3 days before needing a transfusion. Its still not near being under control but 3 days is certainly better than EVERY day!
Sunday, December 2, 2012
The forbidden word...
HOME.
We have been waiting 7 long long weeks to hear the doctors even mention getting B home and they finally have!
I talked with our pediatrician this week and discussed with her that we had been thinking about transferring B. She agreed with us that something needed to change. Apparently, she had been following the case all week and was planning to call us Monday to talk about the possibility of a transfer. She said that if this were her child she would be planning exactly that. She called the hospital and spoke with a few of B's hematology doctors and told them she had recommended a possible transfer and that we were seriously considering it based on the following concerns:
- His primary hematologist has not actual seen him since the week he was admitted.
- Lack of a next step plan or any sense of urgency to come up with one now that they're certain he isn't responding to corticosteroids or IVIG.
- Indifference toward his sky high ferratin levels (excess iron in his body)and the possiblity of transfusion induced iron overload.
- Failure to reach out to other hematology specialists & a perceived reluctance to work collaboratively.
- Brady's quality of life. He has spent all but 3 days of his life in a hospital. We need a plan to get him home!
Within an hour of Dr Miller contacting the doctor's here we got some results. They changed B's primary hematologist to Dr Higman, who has seen him pretty regularly since his admission. I talked with her at length about our concerns. She agreed to get in touch with ANY and AS MANY specialists as we would like and to work collaboratively with them (ie - order any tests they suggests, consider treatments they come up with, etc) to come up with a treatment plan. A ferratin level will be added to his daily labs to monitor how well the desferal is working. And, we now have a set list of goals to achieve in order to get Brady home...
-He must have completed his IV antibiotics. His cultures are negative as of 11/27 and he needs them for 10 days from that date so 12/7 will be his last day.
- He must be requiring 12 hours or less per day of TPN (hyperal & lipid nutrition though his IV) and tolerating tube feeds for a minimum of half his nutritional value. That means 10ml/hr continuous feed.
-Transfusion requirement must space out to about 48 hours between. Then we can come in every other day for outpatient transfusions.
I know it isn't a short list but its something tangible we can work toward. I'm confident we'll get there and I'm hopeful there's a possibility it will be before Christmas. To have our whole family home to celebrate together means more to us than we can put into words! I'm so glad we chose to stand up and advocate. Just the mere mention of a transfer has seemed to make a huge impact. We fully realize it may still come to that but for now, we are willing to give the doctors here another chance!
We have been waiting 7 long long weeks to hear the doctors even mention getting B home and they finally have!
I talked with our pediatrician this week and discussed with her that we had been thinking about transferring B. She agreed with us that something needed to change. Apparently, she had been following the case all week and was planning to call us Monday to talk about the possibility of a transfer. She said that if this were her child she would be planning exactly that. She called the hospital and spoke with a few of B's hematology doctors and told them she had recommended a possible transfer and that we were seriously considering it based on the following concerns:
- His primary hematologist has not actual seen him since the week he was admitted.
- Lack of a next step plan or any sense of urgency to come up with one now that they're certain he isn't responding to corticosteroids or IVIG.
- Indifference toward his sky high ferratin levels (excess iron in his body)and the possiblity of transfusion induced iron overload.
- Failure to reach out to other hematology specialists & a perceived reluctance to work collaboratively.
- Brady's quality of life. He has spent all but 3 days of his life in a hospital. We need a plan to get him home!
Within an hour of Dr Miller contacting the doctor's here we got some results. They changed B's primary hematologist to Dr Higman, who has seen him pretty regularly since his admission. I talked with her at length about our concerns. She agreed to get in touch with ANY and AS MANY specialists as we would like and to work collaboratively with them (ie - order any tests they suggests, consider treatments they come up with, etc) to come up with a treatment plan. A ferratin level will be added to his daily labs to monitor how well the desferal is working. And, we now have a set list of goals to achieve in order to get Brady home...
-He must have completed his IV antibiotics. His cultures are negative as of 11/27 and he needs them for 10 days from that date so 12/7 will be his last day.
- He must be requiring 12 hours or less per day of TPN (hyperal & lipid nutrition though his IV) and tolerating tube feeds for a minimum of half his nutritional value. That means 10ml/hr continuous feed.
-Transfusion requirement must space out to about 48 hours between. Then we can come in every other day for outpatient transfusions.
I know it isn't a short list but its something tangible we can work toward. I'm confident we'll get there and I'm hopeful there's a possibility it will be before Christmas. To have our whole family home to celebrate together means more to us than we can put into words! I'm so glad we chose to stand up and advocate. Just the mere mention of a transfer has seemed to make a huge impact. We fully realize it may still come to that but for now, we are willing to give the doctors here another chance!
Wednesday, November 28, 2012
Busy Day
Lots going on so far today...
Right now B is starting his third IVIG infusion. It will run over the next five hours. Once that is finished he'll head back to the OR to have another PICC line placed. He needs a second line because he basically has a traffic jam of IV needs: TPN nutrition, blood transfusions, IV meds, IVIG, pain management, and chelation therapy. Last night and this morning he received all of his two month vaccines and tolerated them very well. Tonight he will get his first dose of the chelation medication. He'll then get that every night from here on until he is no longer transfusion dependant & taking on iron.
Dr Daniels came in this morning and said they had heard back from two of the hematologist they reached out to to consult on B. One suggested an immunosupressive therapy with a medication called Rituximab. It would suppress his B cell immune response and basically reset his immune system with the hope that once "reset" he would stop hemolyzing. During treatment, and for six months following, he would be particularly susceptible to a specific type of pneumonia -- pneumocyctis pneumonia or PCP -- so he would need to be on a strong IV antibiotic called pentamidine. The other suggestion was to remove his spleen, which is a primary site for red blood cell hemolysis. The hematology team will meet this week to discuss these options and they're also hoping to hear back from a few other hematologists.
Oh, and if you look up toward the top of the blog you'll find a new tab called "Quick Reference". This summarizes B's medical history, meds, docs, etc. Feel free to check it out!

Right now B is starting his third IVIG infusion. It will run over the next five hours. Once that is finished he'll head back to the OR to have another PICC line placed. He needs a second line because he basically has a traffic jam of IV needs: TPN nutrition, blood transfusions, IV meds, IVIG, pain management, and chelation therapy. Last night and this morning he received all of his two month vaccines and tolerated them very well. Tonight he will get his first dose of the chelation medication. He'll then get that every night from here on until he is no longer transfusion dependant & taking on iron.
Dr Daniels came in this morning and said they had heard back from two of the hematologist they reached out to to consult on B. One suggested an immunosupressive therapy with a medication called Rituximab. It would suppress his B cell immune response and basically reset his immune system with the hope that once "reset" he would stop hemolyzing. During treatment, and for six months following, he would be particularly susceptible to a specific type of pneumonia -- pneumocyctis pneumonia or PCP -- so he would need to be on a strong IV antibiotic called pentamidine. The other suggestion was to remove his spleen, which is a primary site for red blood cell hemolysis. The hematology team will meet this week to discuss these options and they're also hoping to hear back from a few other hematologists.
Oh, and if you look up toward the top of the blog you'll find a new tab called "Quick Reference". This summarizes B's medical history, meds, docs, etc. Feel free to check it out!

Tuesday, November 27, 2012
Lots going on
Sorry I haven't posted since Saturday. I attempted it yesterday but B was pretty fussy all day. Anyway...
Brady's blood culture results were not good. He has two infections going on. His PICC has an enterobacter infection and his IJ is positive for staph. He is now on vancomycin for the staph infection and ceftriaxone for the enterobacter. Luckily, they think they caught the infections early before they spread to his bloodstream. He hasn't had any more fevers since Saturday so that's a good sign.
He is still in some pain from the surgery but his incision and G tube site are healing very nicely and he is tolerating his feeds well. He is up to a continuous feed of 10ml per hour. He was weighed yesterday and was down to 2.91 kilos from 3.0 so they are starting TPN nutrition to supplement him until they can get him to full feeds (20ml an hour). Once he is tolerating full continuous feeds then we can start attempting some bottle feeds combined with a bolus feed.
From a heme standpoint, he is back to requiring daily transfusions and on Sunday he actually needed two transfusions because his counts dropped so low. Tomorrow he will get another IVIG treatment and Dr Ambrusco said he is going to reach out to some other hematologists around the country (specifically one at Cincinnati Children's & one at Texas Children's) to see if anyone may have a better idea of what is going on with Brady. When I spoke with heme this morning they told me they are concerned about transfusion-related iron overload. When a person receives chronic blood transfusions they take in excess iron. The body has no way of eliminating this excess iron on its own and it builds up in various organs like the heart, lungs, and liver. If left untreated these build ups cause major problems and can even lead to organ failure. They are going to start daily chelation therapy on B today, using a medication called Desferal, which will allow his body to eliminate the excess iron. It's necessary but scary because it comes with the risk of some significant side effects: joint pain, muscle pain/tenderness, bone problems, fever, headache, nausea, hives, stunted growth, and injection site reactions are all fairly common. Also, the chelation is done over a very long time frame -- between 12 & 14 hours typically -- so he will spend most of his day hooked up to an infusion pump. This creates a problem for B. On Saturday he pulled his IJ half out and they had to remove it. So he is down to one access line, the PICC. But he uses his PICC for IV medications, IVIG, and blood transfusions. Now he also needs continuous TPN and nearly continuous chelation meds so they will have to place at least one additional line, possibly two.
Respiratory wise he is doing very well. He is still on 2 liters of oxygen but he is maintaining a normal respiratory rate which is awesome! I haven't seen anyone from long center since last week so I'm not sure if they plan to wean down further on the oxygen or of 2 liters will be his regular requirement.
Through all of this I'm trying to just take it in stride, one day at a time. But the longer this goes on without answers the harder it gets. I just want my baby to have a chance to get to know a life that doesn't revolve around one procedure, medication, and assessment after another. I want him to know what it's like to be home with his family. If the IVIG therapy isn't helping him I just don't know where things go from there. I've been doing some research myself trying to figure out if there is anyone out there or any hospital that might be able to help my sweetheart. At this point, from what I've read, Texas Children's is the front runner. They have one of the top pediatric hematology/oncology units internationally. So now I keep going around and around in my head, do we try to take him someplace else or continue to have faith in the doctors here? Even if we did want to have him seen someplace else, how do we go about doing that? Do we even have that right? Logistically, how would it be done and would insurance cover a transfer?? My mind is overloaded and I don't know where to turn for those answers. I'm not sure if there is someone on staff at the hospital who handles this kind of situation or if they would even be helpful. If anyone has any thoughts or information please share!!!
Brady's blood culture results were not good. He has two infections going on. His PICC has an enterobacter infection and his IJ is positive for staph. He is now on vancomycin for the staph infection and ceftriaxone for the enterobacter. Luckily, they think they caught the infections early before they spread to his bloodstream. He hasn't had any more fevers since Saturday so that's a good sign.
He is still in some pain from the surgery but his incision and G tube site are healing very nicely and he is tolerating his feeds well. He is up to a continuous feed of 10ml per hour. He was weighed yesterday and was down to 2.91 kilos from 3.0 so they are starting TPN nutrition to supplement him until they can get him to full feeds (20ml an hour). Once he is tolerating full continuous feeds then we can start attempting some bottle feeds combined with a bolus feed.
From a heme standpoint, he is back to requiring daily transfusions and on Sunday he actually needed two transfusions because his counts dropped so low. Tomorrow he will get another IVIG treatment and Dr Ambrusco said he is going to reach out to some other hematologists around the country (specifically one at Cincinnati Children's & one at Texas Children's) to see if anyone may have a better idea of what is going on with Brady. When I spoke with heme this morning they told me they are concerned about transfusion-related iron overload. When a person receives chronic blood transfusions they take in excess iron. The body has no way of eliminating this excess iron on its own and it builds up in various organs like the heart, lungs, and liver. If left untreated these build ups cause major problems and can even lead to organ failure. They are going to start daily chelation therapy on B today, using a medication called Desferal, which will allow his body to eliminate the excess iron. It's necessary but scary because it comes with the risk of some significant side effects: joint pain, muscle pain/tenderness, bone problems, fever, headache, nausea, hives, stunted growth, and injection site reactions are all fairly common. Also, the chelation is done over a very long time frame -- between 12 & 14 hours typically -- so he will spend most of his day hooked up to an infusion pump. This creates a problem for B. On Saturday he pulled his IJ half out and they had to remove it. So he is down to one access line, the PICC. But he uses his PICC for IV medications, IVIG, and blood transfusions. Now he also needs continuous TPN and nearly continuous chelation meds so they will have to place at least one additional line, possibly two.
Respiratory wise he is doing very well. He is still on 2 liters of oxygen but he is maintaining a normal respiratory rate which is awesome! I haven't seen anyone from long center since last week so I'm not sure if they plan to wean down further on the oxygen or of 2 liters will be his regular requirement.
Through all of this I'm trying to just take it in stride, one day at a time. But the longer this goes on without answers the harder it gets. I just want my baby to have a chance to get to know a life that doesn't revolve around one procedure, medication, and assessment after another. I want him to know what it's like to be home with his family. If the IVIG therapy isn't helping him I just don't know where things go from there. I've been doing some research myself trying to figure out if there is anyone out there or any hospital that might be able to help my sweetheart. At this point, from what I've read, Texas Children's is the front runner. They have one of the top pediatric hematology/oncology units internationally. So now I keep going around and around in my head, do we try to take him someplace else or continue to have faith in the doctors here? Even if we did want to have him seen someplace else, how do we go about doing that? Do we even have that right? Logistically, how would it be done and would insurance cover a transfer?? My mind is overloaded and I don't know where to turn for those answers. I'm not sure if there is someone on staff at the hospital who handles this kind of situation or if they would even be helpful. If anyone has any thoughts or information please share!!!
Saturday, November 24, 2012
The good & the bad
Mixed news this morning...
The good: Brady's hemoglobin this morning is 9.0 (from 8.2 yesterday) -- that means for the very first time in his life B's hemoglobin went UP all on its own! Absolutely incredible and definitely a cause for hope.
The bad: After an extremely fussy night with barely any sleep, B woke up with a high fever of 103.4. His labs also came back with elevated white blood cells. Looks like he has some kind of infection going on. They took blood cultures from both his central lines. Surgery will be coming to look at his incision and make sure that isn't showing signs of infection. He may possibly need a spinal tap to check for meningitis. They're starting ceftriaxone now.
The good: Brady's hemoglobin this morning is 9.0 (from 8.2 yesterday) -- that means for the very first time in his life B's hemoglobin went UP all on its own! Absolutely incredible and definitely a cause for hope.
The bad: After an extremely fussy night with barely any sleep, B woke up with a high fever of 103.4. His labs also came back with elevated white blood cells. Looks like he has some kind of infection going on. They took blood cultures from both his central lines. Surgery will be coming to look at his incision and make sure that isn't showing signs of infection. He may possibly need a spinal tap to check for meningitis. They're starting ceftriaxone now.
Friday, November 23, 2012
First Thanksgiving & making moves...
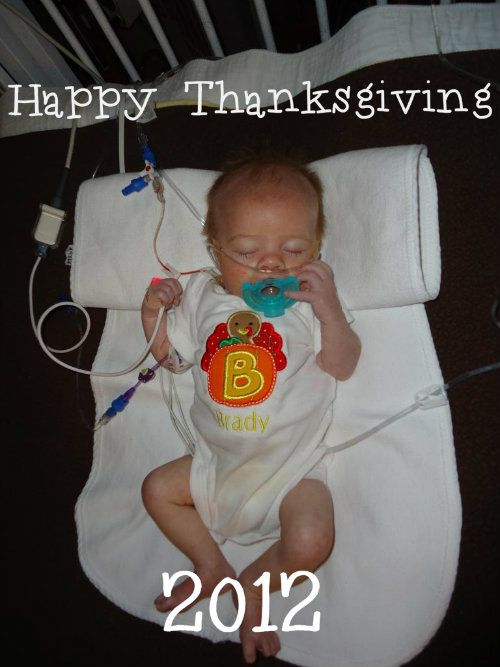
Check out my friend Tiffany's shop at BohemianBabyCouture
Today was kind of a big deal for Brady -- he got a new "home". They moved him out of intensive care and onto the hematology unit. Here's a little photo tour of our little piece of the world...
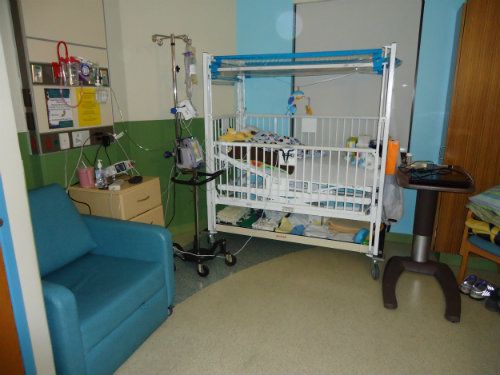

B's bed :)

Mommy's bed (Looks comfy right? Ha!)

It's not much to look at but hey, its more private than the ICU & definitely quieter!! I do miss the huge room we had when he was on the respiratory unit though.
In other news...
B hasn't required a transfusion since wednesday so that's good. His hemoglobin was down today though so I wouldn't be surprised if he gets one tomorrow. I'm hoping tomorrow's retic count will be back up after his IVIG wednesday -- fingers crossed!!! B started taking very small continuous formula feeds through his brand new G tube on Thanksgiving: not quite turkey dinner but something is definitely better than nothing right? lol... So far he is tolerating them very well and the Nissen wrap seems to be working to control his reflux. He has a normal respiratory rate for the first time since he was born. That is amazing!


Tuesday, November 20, 2012
Surgery Day
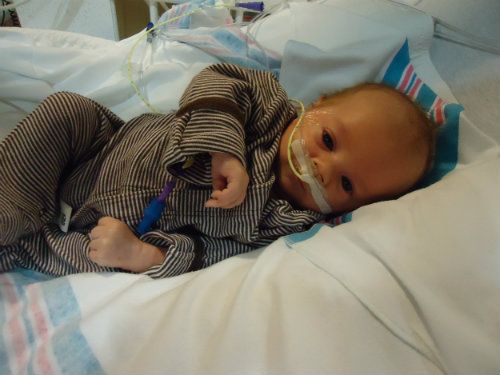
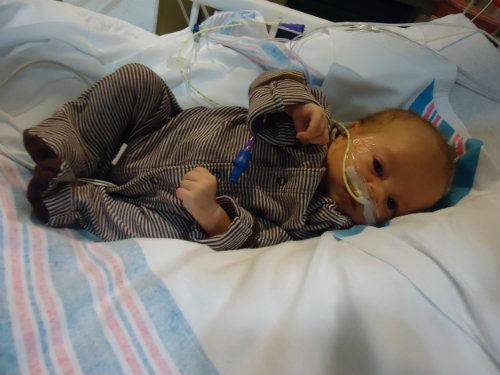
At 9:20 this morning they wheeled our Brady off to the operating room. I've known since last week that surgery was coming. I've wanted this surgery for him. I know it will be best for him in the long run. But, watching them take away your tiny baby is heartbreaking. I think the two and a half hours B was in the operating room were the longest of my life. Thankfully, everything went very well and exactly according to plan. He tolerated surgery and anesthesia without any problems. They decided it would be best to leave him sedated and on the ventilator for the night through the worst of the pain. They're planning to extubate him tomorrow. His tummy is so tiny that the dressing covering his incision covers his whole belly. Their managing his pain with morphine and promise to make sure he's as comfortable as possible while he heals. If all goes well they will start with very small & slow tube feeding tomorrow and see how he does. I feel so terrible for my peanut. He's so little and he's already been through so very much in his short eight weeks. I don't want him to have to feel any pain. I try to find comfort in knowing he will not remember any of this when he is older. Thank God for that!
Before surgery . . .

Post Op . . .
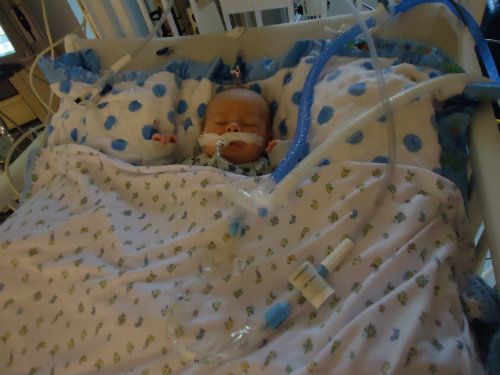
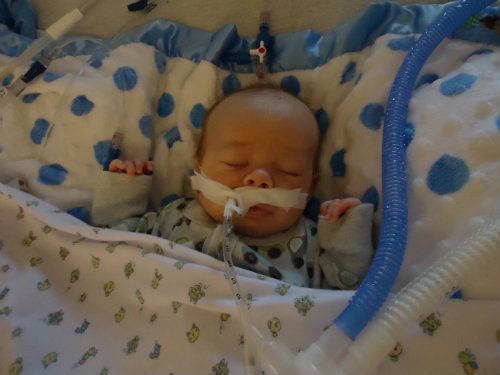
Saturday, November 17, 2012
Could it be working?
praying so very hard right now
Friday, November 16, 2012
Surgery is set
Just spoke with the surgical attending and Brady is scheduled for surgery Tuesday morning at 10:30. He will be having a Nissen Wrap done and a gastric tube ("G tube) put in place. The operation will take about three hours and he will need to be intubated. It's scary that he will be having surgery but I am relieved that this is one issue of his that can be fixed. Feeding will no longer be a struggle and he won't be so uncomfortable from constant refluxing. I have faith that with everyone's prayers and support the surgery will go well and B will be one step closer to home!
Still no answers...
The doctors still struggle to understand what is causing B's anemia and how to treat him. After two complete exchange transfusions they decided they weren't helping and they needed to move on to another treatment. Yesterday Brady had his first IVIG treatment. It went in over the course of about 7 hours. So far, it hasn't had any impact. He needed a blood transfusion this morning for a hemoglobin of 6.4. But, when I asked on rounds the hematologist said that it could take a few days to be effective. If there was no change by monday then they would feel it hasn't worked. So, please pray that this IVIG is the answer we've been waiting for!
B also had an upper GI series yesterday. It was the first step to get him set up for a G tube and possible Nissen Wrap. Brady does eat by mouth but not enough to meet his nutritional needs so a G tube is a definite. I'm waiting to speak with surgery myself but based on their notation in his chart it looks like he could be scheduled for surgery as early as monday or tuesday. It will be up to Dr Sheehan (B's pulmonologist) and the surgical attending to decide whether or not he will get the Nissen done also. Its scary to think that he could be having surgery in just a few days but I also know that getting it done is a step toward home. It would be incredibly frustrating to get his anemia to a point where he could be discharged only to be held up waiting for G tube surgery because he doesn't eat enough on his own.
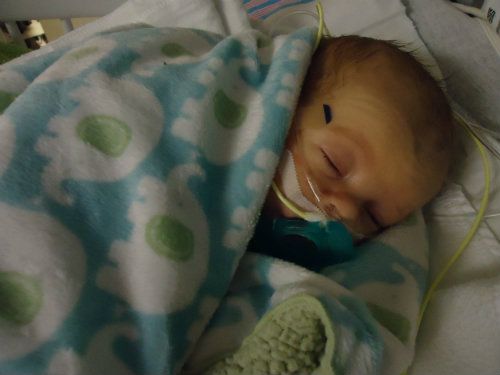


B also had an upper GI series yesterday. It was the first step to get him set up for a G tube and possible Nissen Wrap. Brady does eat by mouth but not enough to meet his nutritional needs so a G tube is a definite. I'm waiting to speak with surgery myself but based on their notation in his chart it looks like he could be scheduled for surgery as early as monday or tuesday. It will be up to Dr Sheehan (B's pulmonologist) and the surgical attending to decide whether or not he will get the Nissen done also. Its scary to think that he could be having surgery in just a few days but I also know that getting it done is a step toward home. It would be incredibly frustrating to get his anemia to a point where he could be discharged only to be held up waiting for G tube surgery because he doesn't eat enough on his own.



Wednesday, November 14, 2012
38 days
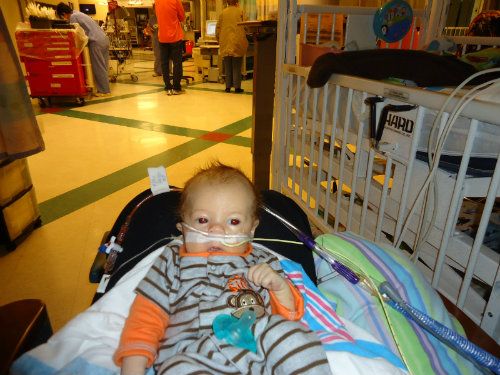
Yesterday they gave B another exchange transfusion. They were hoping maybe a second transfusion would give him a sustained recovery from the hemolysis. But, this morning his hemoglobin is already down to 8.9 from 11.4 last night. Looks like it didn't work, even temporarily. Now they're talking about starting IVIG on him tomorrow. They aren't sure if that will help either but they feel it's worth a shot. It's so frustrating that they still don't really know what is going on or how to help him and the more frequently he is transfused the more problems that can stem from the transfusions. He now gets something called a feratin test every week because iron builds up in the organs of patients receiving frequent transfusions and iron build up an cause other issues. Due to the hemolysis they also have to monitor his bilirubin levels closely to make sure he isn't jaundice.
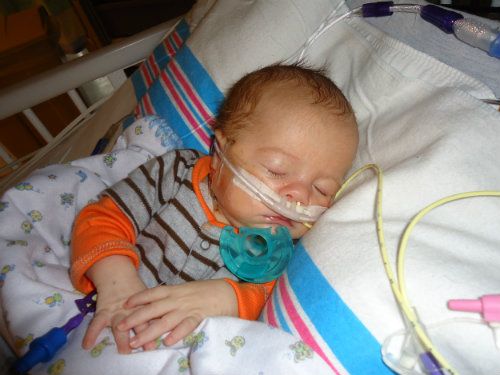
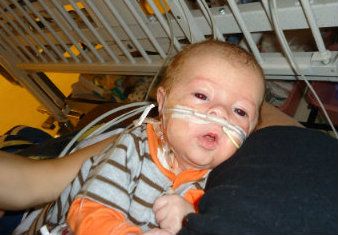
In the good news department he is doing better from a respiratory standpoint. They are switching him from High Flow oxygen to a regular nasal cannula this afternoon. He also started bottle feeding again yesterday and is taking feeds pretty well so far. He still has a long way to go before he wouldn't need his tube feeds but it's a step forward.
These days I'm all about small victories!
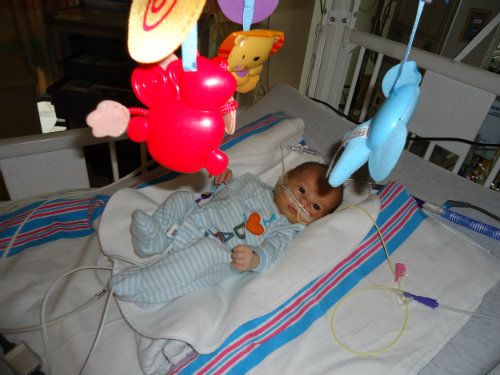
Sunday, November 11, 2012
A new high!
Not much to report today but...B's retic count today was 104 -- an all time high and exactly what they would expect to see in a baby with anemia. The hematology team believes the exchange transfusion made a fairly significant difference for him but since he is still hemolyzing and requiring transfusions daily they're talking about repeating it again later in the week.


Friday, November 9, 2012
A step in the right direction...
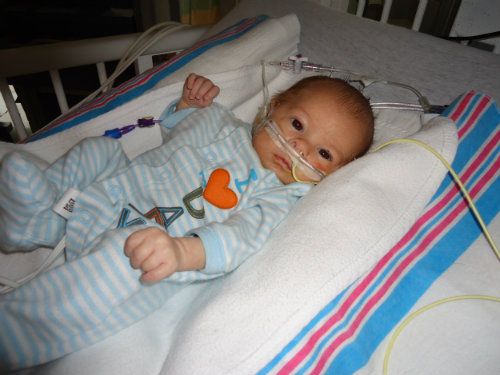
This was Brady this morning...
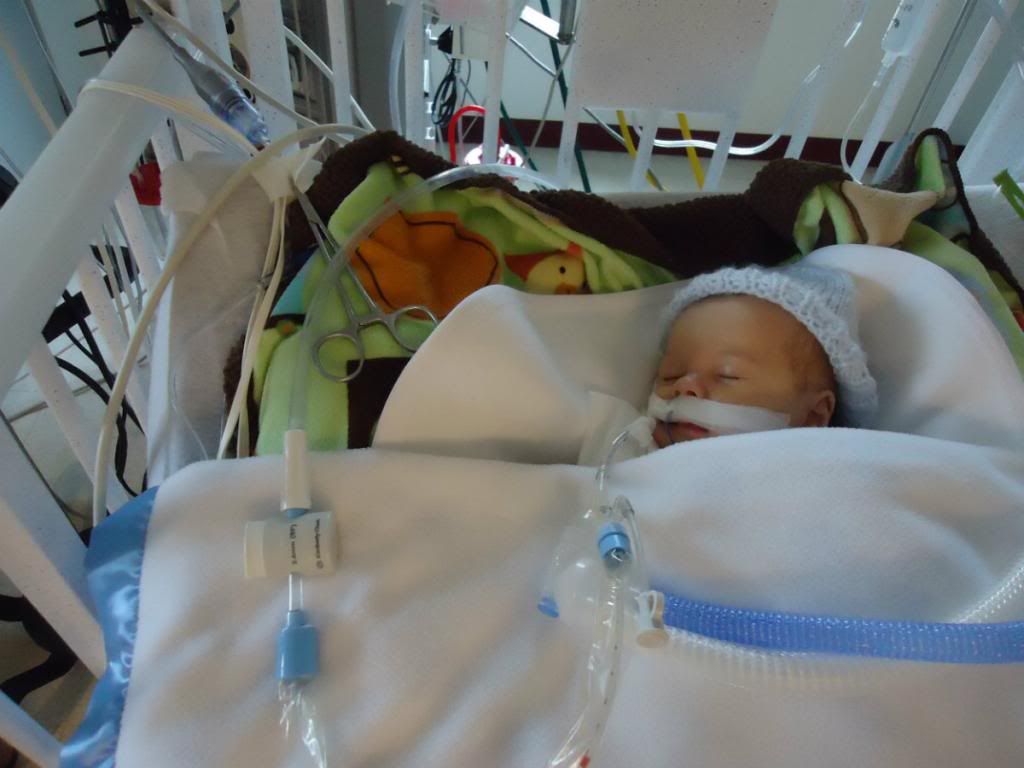
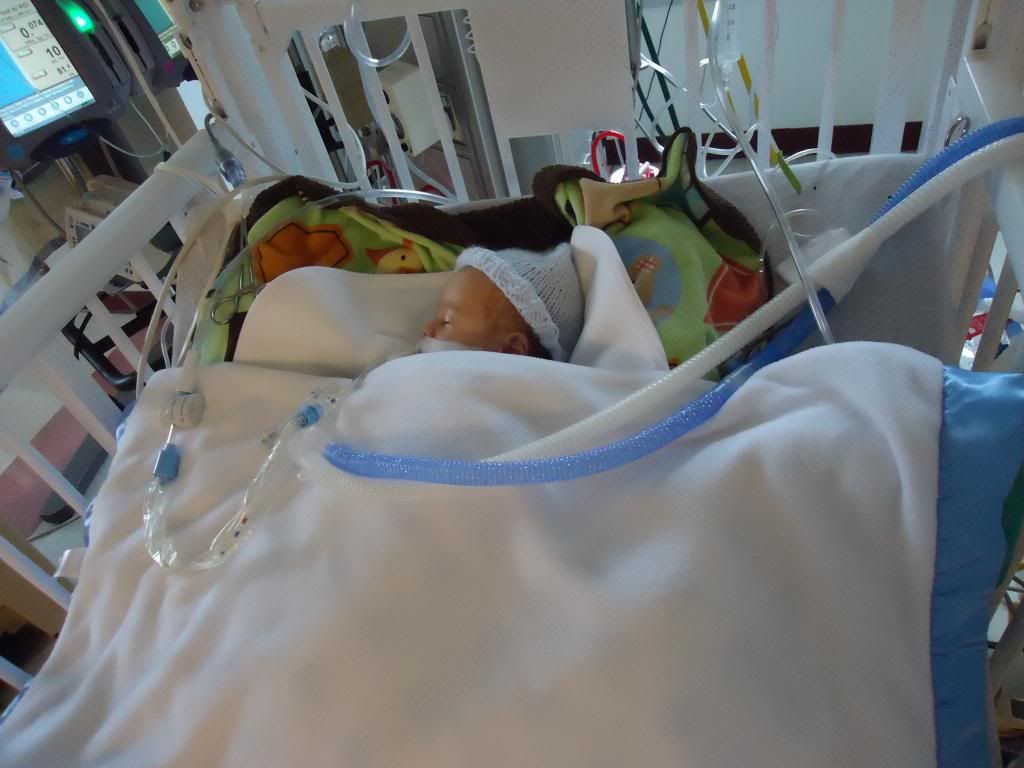
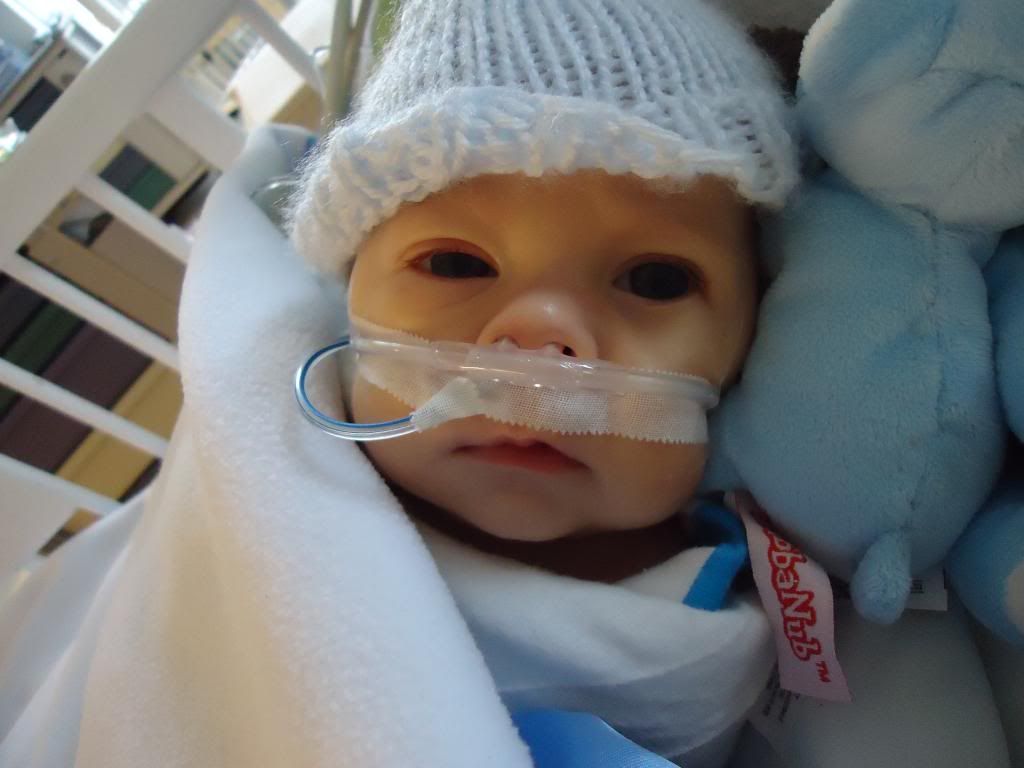
And here is Brady now!
Brady came off the vent -- yay!! He was showing moderate retractions and was very tachypnic (respirations in the 100's) so he is on High Flow oxygen for today to help him transition but he should be back on his regular nasal canula sometime tomorrow. Dr Ambrusco from Hematology came in this afternoon. Brady's hemoglobin level was 9.8 this morning, which is down from 12.6 yesterday, but he isn't concerned. He said we can expect to see his hemoglobin drop. What matters is whether or not his bone marrow kicks in and compensates for the anemia. So far, that looks promising. Reticulocytes are baby red blood cells. Brady's reticulocyte count (aka retic count) has never been higher than 36 before and is usually only in the single digits. A normal retic count in a healthy baby his age would be between 30 & 90. In a patient with anemia the retic count should be elevated, meaning the body recognizes the anemia and is attempting to fix it. This morning B's retic count was 47, a new high for him. It shows that his bone marrow is starting to make more reticulocytes as his hemoglobin drops and that's exactly what its supposed to do! It's still too early to say for sure whether or not the exchange transfusion worked but for now it's looking positive :)
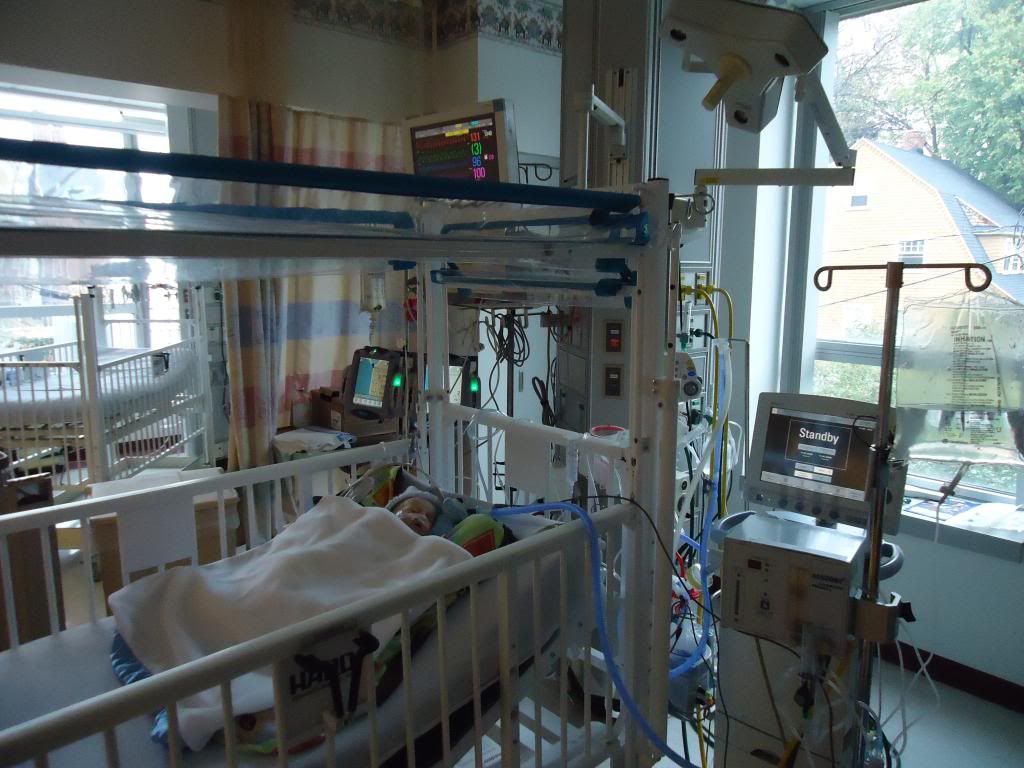
Brady's ICU room
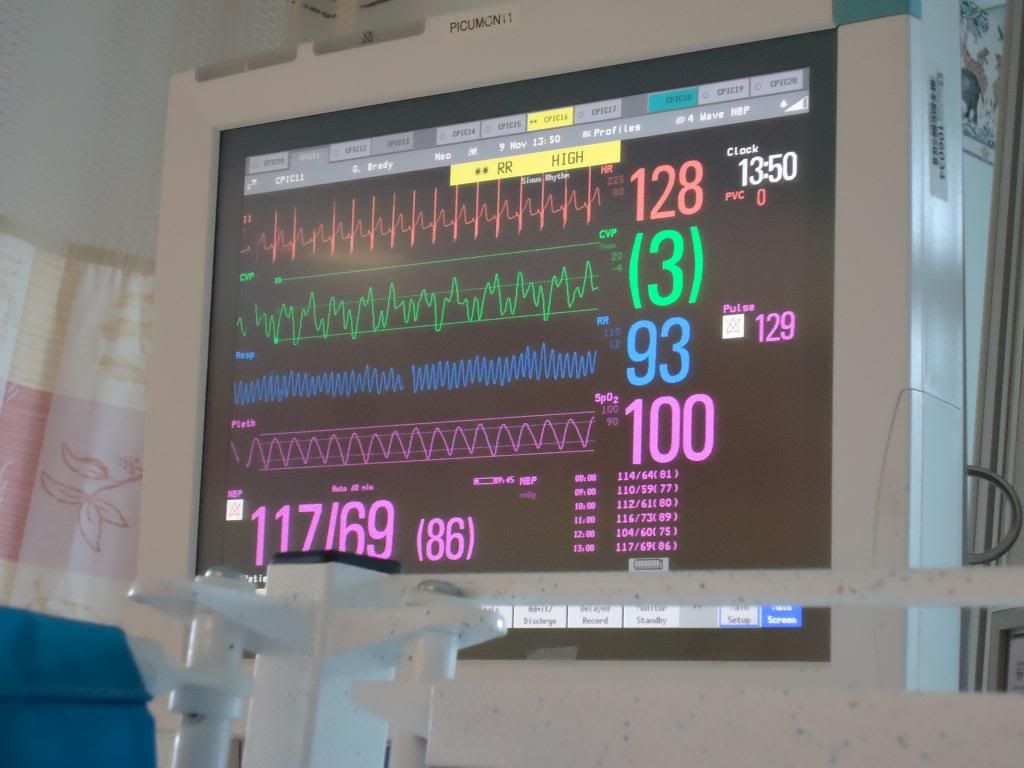
His monitor, which shows his heart rate (red), veinous pressure (green), respiratory rate (blue), and oxygen saturation (pink)
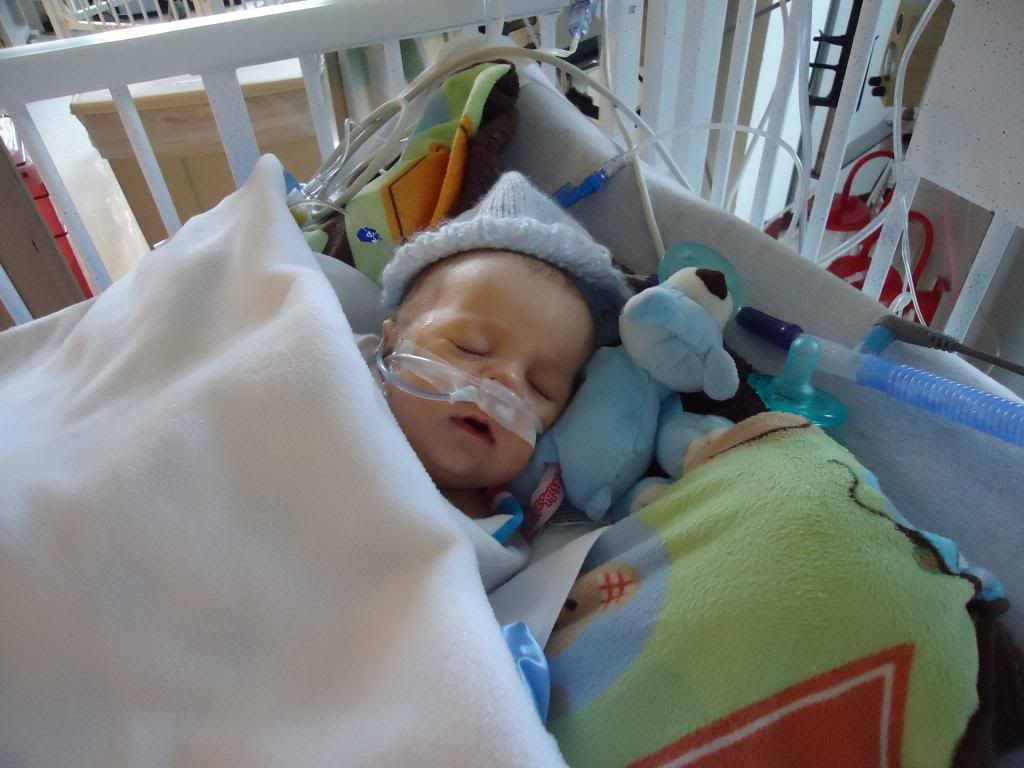
B -- snug as a bug!


And here is Brady now!

Brady came off the vent -- yay!! He was showing moderate retractions and was very tachypnic (respirations in the 100's) so he is on High Flow oxygen for today to help him transition but he should be back on his regular nasal canula sometime tomorrow. Dr Ambrusco from Hematology came in this afternoon. Brady's hemoglobin level was 9.8 this morning, which is down from 12.6 yesterday, but he isn't concerned. He said we can expect to see his hemoglobin drop. What matters is whether or not his bone marrow kicks in and compensates for the anemia. So far, that looks promising. Reticulocytes are baby red blood cells. Brady's reticulocyte count (aka retic count) has never been higher than 36 before and is usually only in the single digits. A normal retic count in a healthy baby his age would be between 30 & 90. In a patient with anemia the retic count should be elevated, meaning the body recognizes the anemia and is attempting to fix it. This morning B's retic count was 47, a new high for him. It shows that his bone marrow is starting to make more reticulocytes as his hemoglobin drops and that's exactly what its supposed to do! It's still too early to say for sure whether or not the exchange transfusion worked but for now it's looking positive :)
Brady's ICU room

His monitor, which shows his heart rate (red), veinous pressure (green), respiratory rate (blue), and oxygen saturation (pink)

B -- snug as a bug!

Thursday, November 8, 2012
A new beginning?
Brady finally got his plasma exchange transfusion overnight last night. He tolerated it well and so far his hemoglobin has been very stable. Post transfusion, about 5 am, his hemoglobin was 13.1 and at 5 pm it was holding strong at 12.6 -- 12 hours with almost no change!! That is incredible for B considering he's been needing transfusions less than 24 hours apart the last few days. I am daring to hope that maybe this is his turning point toward home. Hope. Its scary to let myself feel hopeful but I am thinking positive thoughts.
He is still on the vent for now. They stopped his fentanyl sedation at 2pm and had planned to extubate him but he had an episode where his respirations & sats dropped so they put it off. Then they tried at about 5:00 but when they disconnected the vent he didn't initiate any breaths so they said he wasn't ready and reconnected it. Now, he just had two desats and didn't initiate breaths (meaning he waited for the vent to breathe for him) so they're thinking he may need more time before being extubated. :(
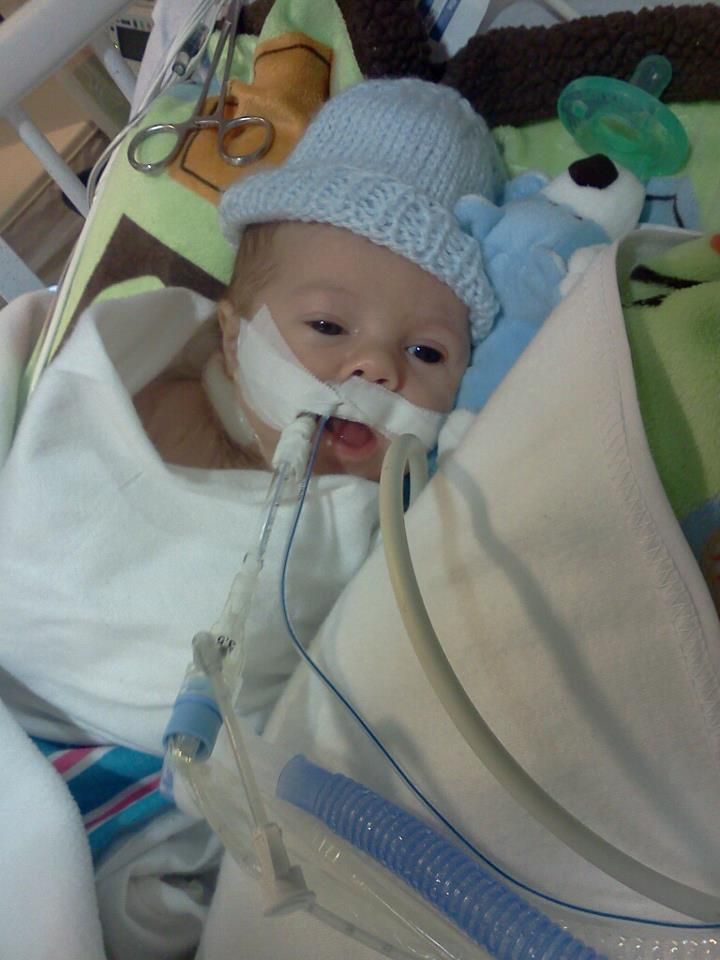
He is still on the vent for now. They stopped his fentanyl sedation at 2pm and had planned to extubate him but he had an episode where his respirations & sats dropped so they put it off. Then they tried at about 5:00 but when they disconnected the vent he didn't initiate any breaths so they said he wasn't ready and reconnected it. Now, he just had two desats and didn't initiate breaths (meaning he waited for the vent to breathe for him) so they're thinking he may need more time before being extubated. :(

Wednesday, November 7, 2012
Playing catch up...
I'm starting this blog mostly as a place to keep our family & friends up to speed on how our sweet little fighter is doing. I also hope this will serve as a place to put all the thoughts and memories of this crazy journey so that we will have a record to look back on. So, I'll start from the beginning...
We found out we were expecting our fourth child just a week before our son Ethan's First Birthday. We were overjoyed! At my first prenatal appointment we were told our newest addition was due to arrive on October 30th. As it turns out, Brady had other plans. After battling with preterm labor starting at around 23 weeks, multiple nights in the hospital, beta shots for baby's lungs, and weekly doctors appointments we made it to 35 weeks exactly.

That morning - Tuesday September 25, 2012 - I was having lots of contractions, which was typical, so I went about my normal day. Tim was working days. By the time he got home just before 3:30 I knew this time was different. We dropped the kids off with his parents and headed to Children's. We got to the hospital around 5:30 pm but they didn't have any rooms available. I labored in the waiting room until 7 when they finally brought me back and gave me a bed in the OR recovery bay -- where 5 other women were already laboring!! They got me settled on a monitor and Dr Farkash examined me. He said I was dilated 4-5 and 90%. They placed a heplock and let me walk around. I walked the L&D floor from 7:30 until just after 9. At that point I was feeling weak and unsteady during contractions and couldn't talk through them so I decided I should get rechecked. At 9:30 I was 8cm and 100% and by just after 10 I was complete and being wheeled to an OR to deliver (since there were still NO delivery rooms open!). Brady Timothy Getty came into the world at 10:33 pm weighing in at 6 lbs & 9 oz and a tiny 18.5 inches long. We didn't know what the babies gender was and were thrilled to have another little boy! But our joy quickly turned to concern...
Brady was born very very sick. He had a condition known as hydrops which made him extremely pale, swollen, and lethargic. He barely made a cry. I held my tiny new son for just a few minutes before they whisked him away to the NICU :(



During his first 48 hours of life B required two blood transfusions and a platelet transfusion to save his life. He was on a ventilator to breathe for him. As they were able to treat the hydrops things started to get better quickly. He only needed the vent for 3 days and after just 9 days in the NICU he was discharged! We thought that the whole terrifying ordeal was behind us and we were just happy to have our peanut home where he belongs.




But within days of coming home we could tell that B was in trouble again. He came home around dinner time on Thursday the 4th and Monday morning, the 8th, he was rushed by ambulance from his pediatricians office back to Children's in respiratory failure. When we arrived in the ER he was unable to breathe on his own, hypothermic, in kidney failure, and life threateningly anemic. My little boy's teeny body was shutting down. He was intubated and stabilized and admitted to the PICU (pediatric intensive care unit). He spent six days on the vent and seven days on a RAM canula, before being switched to regular oxygen. During this time he was requiring blood transfusions about every five days but doctors couldn't determine why. He had surgery on 10/19. They did a bone marrow biopsy & aspiration, and a bronchoscopy & BAL. B was diagnosed with Surfactant Protein-C deficiency and we were told his bone marrow was not working properly. He fails to make RBC's at a normal rate and his body is also destroying the RBC's in his blood and bone marrow.
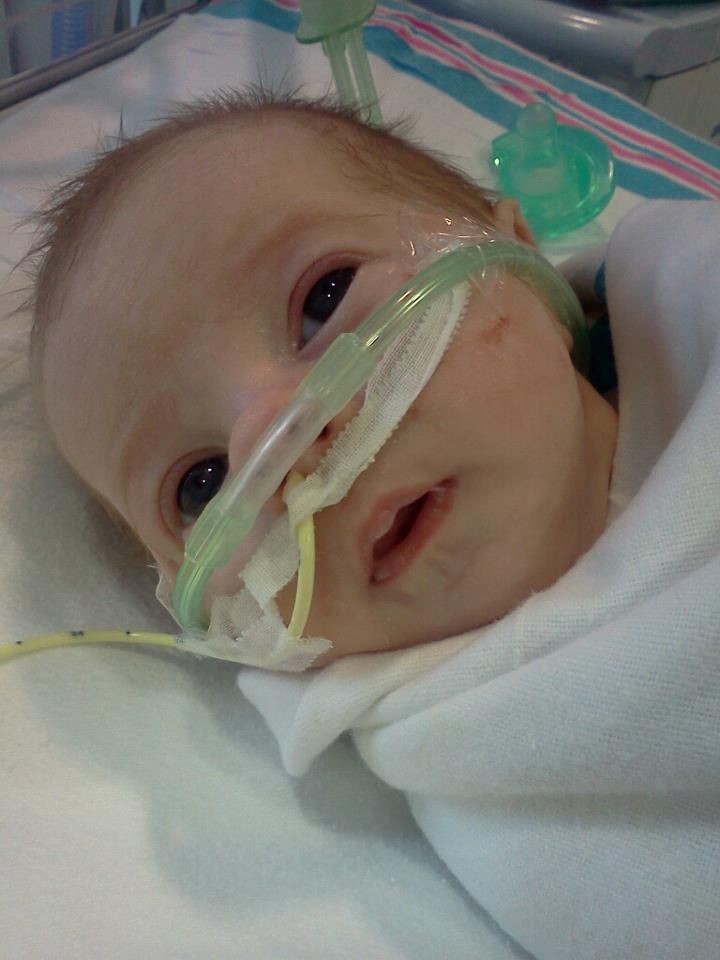
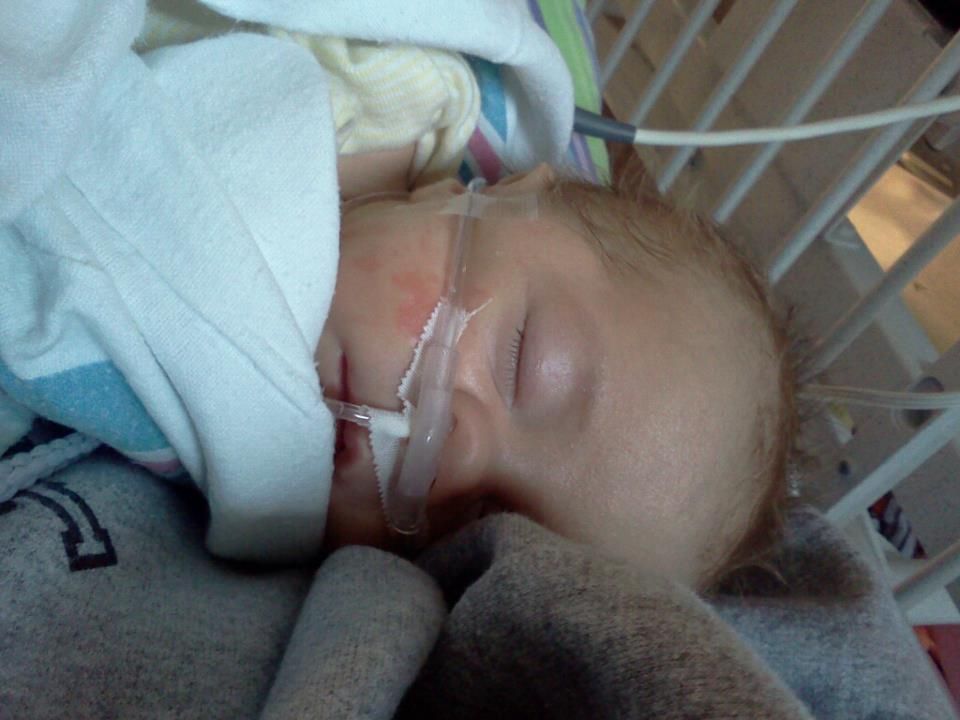
Finally, after 13 days in the PICU Brady was moved up to a regular room. He started eating well and gaining weight. He was doing great on very low oxygen settings. He was tolerating his transfusions well and going nearly a week between them. Then, about a week ago things started to deteriorate. Suddenly B was hemolyzing RBC's at a faster & faster pace. This makes his respiratory status unstable. It also makes him too tired to eat.

On Sunday we were moved back down to the PICU. This last week B was being transfused every third day, then every other, and now he has been getting transfused twice a day because his numbers (how many RBC's show up on a CBC) are falling so rapidly. His hematologists decided that Brady's anemia is out of control and it is time for drastic measures.
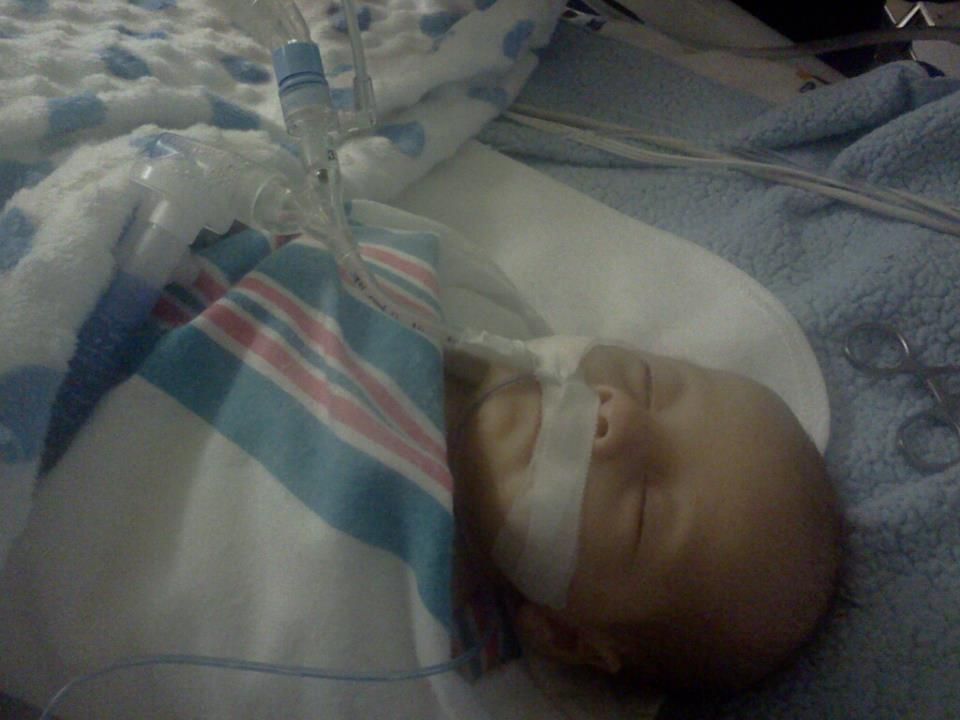

As I type this B is in the OR. They are placing a central line into his femoral artery. After that he will be getting a plasma exchange transfusion. Basically, they are going to completely replace all of the blood in his little body. The hope is that the cause of his anemia is antibodies in his blood. By replacing his blood the antibodies would be eliminated and the anemia would be resolved. Its a scary thought, replacing all his blood, and its not without risks but if we don't do something to help him we could lose our little boy. I'm so scared right now. But I think I'm more afraid that the exchange won't work than I am of the actual procedure. This is the only thing they can think of to help him so what happens if this doesn't fix the problem?
Anyway, once the exchange is finished the next couple of days will reveal whether or not it was successful. If Brady's blood counts remain stable and he is no longer hemolyzing then we will know it worked. Fingers crossed!!!
We found out we were expecting our fourth child just a week before our son Ethan's First Birthday. We were overjoyed! At my first prenatal appointment we were told our newest addition was due to arrive on October 30th. As it turns out, Brady had other plans. After battling with preterm labor starting at around 23 weeks, multiple nights in the hospital, beta shots for baby's lungs, and weekly doctors appointments we made it to 35 weeks exactly.

That morning - Tuesday September 25, 2012 - I was having lots of contractions, which was typical, so I went about my normal day. Tim was working days. By the time he got home just before 3:30 I knew this time was different. We dropped the kids off with his parents and headed to Children's. We got to the hospital around 5:30 pm but they didn't have any rooms available. I labored in the waiting room until 7 when they finally brought me back and gave me a bed in the OR recovery bay -- where 5 other women were already laboring!! They got me settled on a monitor and Dr Farkash examined me. He said I was dilated 4-5 and 90%. They placed a heplock and let me walk around. I walked the L&D floor from 7:30 until just after 9. At that point I was feeling weak and unsteady during contractions and couldn't talk through them so I decided I should get rechecked. At 9:30 I was 8cm and 100% and by just after 10 I was complete and being wheeled to an OR to deliver (since there were still NO delivery rooms open!). Brady Timothy Getty came into the world at 10:33 pm weighing in at 6 lbs & 9 oz and a tiny 18.5 inches long. We didn't know what the babies gender was and were thrilled to have another little boy! But our joy quickly turned to concern...
Brady was born very very sick. He had a condition known as hydrops which made him extremely pale, swollen, and lethargic. He barely made a cry. I held my tiny new son for just a few minutes before they whisked him away to the NICU :(



During his first 48 hours of life B required two blood transfusions and a platelet transfusion to save his life. He was on a ventilator to breathe for him. As they were able to treat the hydrops things started to get better quickly. He only needed the vent for 3 days and after just 9 days in the NICU he was discharged! We thought that the whole terrifying ordeal was behind us and we were just happy to have our peanut home where he belongs.




But within days of coming home we could tell that B was in trouble again. He came home around dinner time on Thursday the 4th and Monday morning, the 8th, he was rushed by ambulance from his pediatricians office back to Children's in respiratory failure. When we arrived in the ER he was unable to breathe on his own, hypothermic, in kidney failure, and life threateningly anemic. My little boy's teeny body was shutting down. He was intubated and stabilized and admitted to the PICU (pediatric intensive care unit). He spent six days on the vent and seven days on a RAM canula, before being switched to regular oxygen. During this time he was requiring blood transfusions about every five days but doctors couldn't determine why. He had surgery on 10/19. They did a bone marrow biopsy & aspiration, and a bronchoscopy & BAL. B was diagnosed with Surfactant Protein-C deficiency and we were told his bone marrow was not working properly. He fails to make RBC's at a normal rate and his body is also destroying the RBC's in his blood and bone marrow.


Finally, after 13 days in the PICU Brady was moved up to a regular room. He started eating well and gaining weight. He was doing great on very low oxygen settings. He was tolerating his transfusions well and going nearly a week between them. Then, about a week ago things started to deteriorate. Suddenly B was hemolyzing RBC's at a faster & faster pace. This makes his respiratory status unstable. It also makes him too tired to eat.

On Sunday we were moved back down to the PICU. This last week B was being transfused every third day, then every other, and now he has been getting transfused twice a day because his numbers (how many RBC's show up on a CBC) are falling so rapidly. His hematologists decided that Brady's anemia is out of control and it is time for drastic measures.


As I type this B is in the OR. They are placing a central line into his femoral artery. After that he will be getting a plasma exchange transfusion. Basically, they are going to completely replace all of the blood in his little body. The hope is that the cause of his anemia is antibodies in his blood. By replacing his blood the antibodies would be eliminated and the anemia would be resolved. Its a scary thought, replacing all his blood, and its not without risks but if we don't do something to help him we could lose our little boy. I'm so scared right now. But I think I'm more afraid that the exchange won't work than I am of the actual procedure. This is the only thing they can think of to help him so what happens if this doesn't fix the problem?
Anyway, once the exchange is finished the next couple of days will reveal whether or not it was successful. If Brady's blood counts remain stable and he is no longer hemolyzing then we will know it worked. Fingers crossed!!!
Subscribe to:
Comments (Atom)








